+200,000 Operations Performed
Prof. Dr. Efekan Coşkunseven Keratoconus & Corneal Diseases
Experience and International Reference Approach in Keratoconus Treatment
Firsts in Turkey and the World
He is a globally recognized authority in keratoconus, whose treatment protocols have served as the foundation for training numerous physicians worldwide.
Corneal Collagen Cross-Linking (CXL)
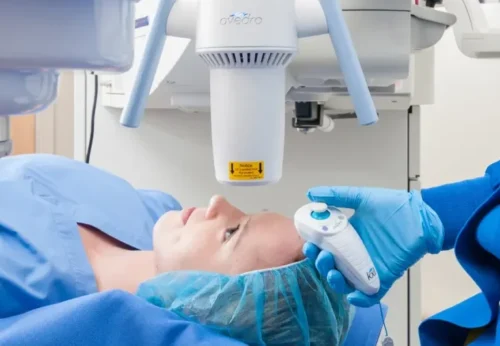 First performed in Turkey in 2004 by Dr. Efekan Coşkunseven, this technique is regarded as a "paradigm shift" in the treatment of keratoconus. Its primary goal is not to correct vision, but to address the underlying biomechanical weakness of the cornea.
First performed in Turkey in 2004 by Dr. Efekan Coşkunseven, this technique is regarded as a "paradigm shift" in the treatment of keratoconus. Its primary goal is not to correct vision, but to address the underlying biomechanical weakness of the cornea.
Which conditions is it used for?
Cross-linking is used primarily to halt the progression of keratoconus, but it can also be applied in pellucid marginal degeneration (PMD) — a variant of keratoconus — and in cases of ectasia that develop following excimer laser surgery. In addition, it may be used as a preventive measure in patients with very thin corneas who wish to undergo excimer laser treatment, in order to reduce the risk of post-operative ectasia.
The Core Philosophy of Treatment
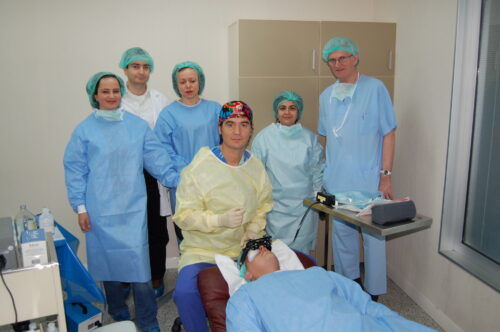 All leading health authorities unanimously agree that this treatment is the only method proven to halt the progression of the disease. The procedure works by strengthening existing bonds between collagen fibers — the cornea's primary structural component — and forming new ones (cross-links).
All leading health authorities unanimously agree that this treatment is the only method proven to halt the progression of the disease. The procedure works by strengthening existing bonds between collagen fibers — the cornea's primary structural component — and forming new ones (cross-links).
Protecting Your Eyes Through Early Diagnosis Secures Your Vision for the Future.
Although keratoconus is a condition that threatens vision over time, modern treatment approaches now make it possible to bring the disease under control.
Cross-linking stands out as an effective treatment option that strengthens the cornea and slows the progression of the disease.
Do not neglect your routine eye examinations.
Early diagnosis is always the most effective treatment.
Protocols: Epi-off (Classic) and Epi-on (Transepithelial)
- Epi-off (Epithelium Removed): This is the original, "gold standard" protocol for the treatment. Specialists note that gently removing the epithelium — the cornea's outermost protective layer — ensures that riboflavin (vitamin B2) penetrates the stromal layer fully and homogeneously. The drawback is that the first 24–48 hours after the procedure tend to be more uncomfortable, and the epithelium requires 3–5 days to regenerate.
- Epi-on (Epithelium Intact): In this newer approach, the epithelium is left in place. Riboflavin is administered using specially formulated drops — with modified concentration or chemical carriers — designed to penetrate the intact epithelium. The advantage is significantly greater post-procedure comfort and a virtually immediate return to daily activities. However, some specialists note that debate continues over whether the riboflavin penetrates deeply enough.
The Role of Riboflavin (Vitamin B2): The riboflavin drops applied act as a photosensitizing agent, penetrating the stromal layer of the cornea.
- The Effect of UV-A: The controlled UV-A light activates the riboflavin, triggering the formation of free radicals — particularly singlet oxygen. These high-energy molecules cause new, permanent covalent bonds to form between collagen fibrils.
- The Result: This process effectively reinforces the weak, flexible cornea — as if binding it with "steel cables" — increasing its stiffness and mechanical resistance, and halting its progressive forward bulging.
Post-Treatment Process
 Following the epi-off procedure, the eye is covered with a protective bandage contact lens. Some stinging, tearing, and light sensitivity (photophobia) in the first few days is normal. Patients are prescribed antibiotic and corticosteroid eye drops. One important point to be aware of is that vision may temporarily become blurred after CXL. The corneal healing and strengthening process continues for several months, and it may take 1 to 6 months for vision to stabilize.
Following the epi-off procedure, the eye is covered with a protective bandage contact lens. Some stinging, tearing, and light sensitivity (photophobia) in the first few days is normal. Patients are prescribed antibiotic and corticosteroid eye drops. One important point to be aware of is that vision may temporarily become blurred after CXL. The corneal healing and strengthening process continues for several months, and it may take 1 to 6 months for vision to stabilize.
Which Keratoconus Patients Are Suitable Candidates for CXL?
This treatment is most commonly recommended for the following groups of patients:
1. Those in the early or intermediate stages of keratoconus.
2. Those whose vision has not yet deteriorated significantly. 3. Those whose corneal thickness remains within acceptable limits.
4. Cases showing signs of disease progression. In the presence of significant corneal thinning, scar tissue formation, or advanced-stage keratoconus, a different treatment approach may be required.
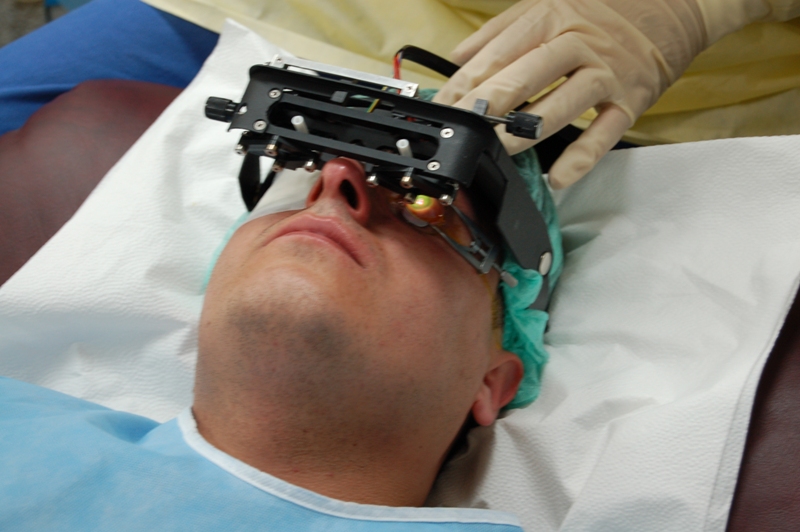
The first CCL device used in Turkey's first CCL treatment (2004)
The Scientific Mechanism of Cross-Linking Treatment
Corneal Cross-Linking (CXL) is a treatment with a strong scientific foundation that directly targets the underlying cause of keratoconus: corneal biomechanical weakness. It is not simply a surface-level application — it is a photochemical reaction that enhances the molecular and structural integrity of the cornea.
In keratoconus, the core problem is not the change in corneal shape itself, but the loosening of the collagen structure and weakening of the connective tissue that causes that change. Cross-linking acts precisely at this level.
Riboflavin (Vitamin B2) + UV-A Light Interaction
The treatment is based on a controlled photochemical reaction between riboflavin and UV-A light.
- The corneal tissue is saturated with riboflavin drops.
- Riboflavin acts as a photosensitizer within the corneal stroma.
- When UV-A light is applied, riboflavin becomes activated.
- The resulting free oxygen radicals promote the formation of new covalent bonds between collagen fibers.
This process takes place directly within the internal architecture of the cornea. In other words, the treatment does not change the shape of the cornea — it changes its mechanical strength.
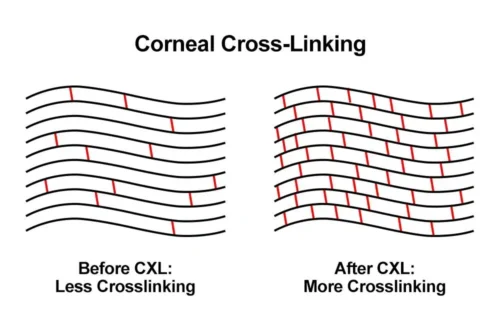
Increase in the Number of Collagen Cross-Links
In a healthy cornea, natural bonds exist between collagen fibers. In keratoconus, the number of these bonds decreases and the fibers loosen.
After cross-linking:
- New chemical bridges form between collagen fibrils
- Interfibrillar sliding is reduced
- The internal architecture of the cornea is reinforced
- Biomechanical stability increases
This halts the progression mechanism of keratoconus at its root.
Changes in Corneal Stiffness and Elastic Modulus
Biomechanical studies have demonstrated that after cross-linking:
- Corneal stiffness can increase by 200–300%
- The elastic modulus (Young's Modulus) rises significantly
- The cornea becomes more resistant to intraocular pressure
- Progressive anterior bulging is halted
These changes begin at the microstructural level, before any topographic improvement becomes visible.
Evidence-Based Efficacy in Scientific Literature
Cross-linking is among the most scientifically well-supported treatments in ophthalmology.
- Long-term follow-up studies spanning 10–15 years have shown that progression is halted in the vast majority of cases
- Its efficacy has been demonstrated even in pediatric patients
- Published data show a significant reduction in the need for corneal transplantation
- Stabilization is clearly observed on Pentacam imaging and biomechanical measurements
When performed at an early stage in particular, CXL has the potential to alter the natural course of the disease.







